Rheumatoid Arthritis and Foot Health
 Rheumatoid arthritis, or RA, is an autoimmune disease that causes inflammation in the joints. In RA, the immune system mistakenly attacks the lining of the joints, causing swelling, pain, and potentially severe joint damage. This can cause problems in any of the 30 foot joints, but it most commonly affects the toes and ankles. RA can also lead to deformities such as bunions, claw toes, or severe flattening of the foot, as well as pain and difficulty walking. Chronic inflammation can weaken the ligaments and tendons in the foot, leading to instability and increased risk of injury. Podiatrists, or foot doctors, can help manage RA-related foot issues by providing targeted treatments. Among them are orthotics to support the joints, advice on proper footwear to reduce stress on the affected areas, and exercises to maintain joint function and mobility. They also monitor for changes or deterioration in foot health that might require more aggressive interventions, including injections or surgery. If you’re a rheumatoid arthritis patient with problems in the feet and ankles, it is suggested that you add a podiatrist to your care team.
Rheumatoid arthritis, or RA, is an autoimmune disease that causes inflammation in the joints. In RA, the immune system mistakenly attacks the lining of the joints, causing swelling, pain, and potentially severe joint damage. This can cause problems in any of the 30 foot joints, but it most commonly affects the toes and ankles. RA can also lead to deformities such as bunions, claw toes, or severe flattening of the foot, as well as pain and difficulty walking. Chronic inflammation can weaken the ligaments and tendons in the foot, leading to instability and increased risk of injury. Podiatrists, or foot doctors, can help manage RA-related foot issues by providing targeted treatments. Among them are orthotics to support the joints, advice on proper footwear to reduce stress on the affected areas, and exercises to maintain joint function and mobility. They also monitor for changes or deterioration in foot health that might require more aggressive interventions, including injections or surgery. If you’re a rheumatoid arthritis patient with problems in the feet and ankles, it is suggested that you add a podiatrist to your care team.
Because RA affects more than just your joints, including the joints in your feet and ankles, it is important to seek early diagnosis from your podiatrist if you feel like the pain in your feet might be caused by RA. For more information, contact one of our podiatrists of Princeton Foot and Ankle Associates. Our doctors will assist you with all of your podiatric concerns.
What Is Rheumatoid Arthritis?
Rheumatoid Arthritis (RA) is an autoimmune disorder in which the body’s own immune system attacks the membranes surrounding the joints. Inflammation of the lining and eventually the destruction of the joint’s cartilage and bone occur, causing severe pain and immobility.
Rheumatoid Arthritis of the Feet
Although RA usually attacks multiple bones and joints throughout the entire body, almost 90 percent of cases result in pain in the foot or ankle area.
Symptoms
- Swelling and pain in the feet
- Stiffness in the feet
- Pain on the ball or sole of feet
- Joint shift and deformation
Diagnosis
Quick diagnosis of RA in the feet is important so that the podiatrist can treat the area effectively. Your doctor will ask you about your medical history, occupation, and lifestyle to determine the origin of the condition. Rheumatoid Factor tests help to determine if someone is affected by the disease.
If you have any questions please feel free to contact our offices located in Princeton, and West Windsor, NJ . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Rheumatoid Arthritis in the Feet
Although rheumatoid arthritis attacks multiple bones and joints throughout the entire body, ninety percent of people who actually develop this condition usually do so in the foot or ankle area. Those who develop this kind of arthritis in the feet usually develop symptoms around the toes and forefeet first, before anywhere else. Rheumatoid arthritis appears to have a genetic component. If it runs in the family, then you will be more likely to develop it as well.
Rheumatoid arthritis is an autoimmune disorder in which the body’s own immune system attacks the lining of the membranes surrounding the joints. This causes inflammation of the membrane lining, and the gradual destruction of the joint’s cartilage and even bone.
Some of the most common symptoms that are associated with RA include pain and swelling of the feet. Stiffness in the feet is also another common symptom that people experience. Those who have RA in the feet usually feel the pain in the ball or sole of their feet. This can get to be very painful at times. A person's joints can even shift and become deformed after a period of time.
In order to properly diagnose RA in the feet it is usually necessary for a doctor or podiatrist to evaluate the area. Your doctor will also question you about your medical history, occupation, etc., to determine whether anything in your lifestyle may have triggered the condition. There are a number of tests that may be performed to help diagnose RA, such as a rheumatoid factor test. There is, however, no one single test that will tell you for sure if you have RA. There are different X-rays that can be taken as well to determine if a person has RA in their feet.
There is a range of treatment options for rheumatoid arthritis. Treatment of RA is usually a lifelong process that includes a variety of methods of treatment and therapy. Your doctor can prescribe special shoes that should help with arch support as well as heel support. A physical therapist can help those with this condition learn exercises which will keep their joints flexible. Surgery may be needed to correct some of the issues with the feet, such as bunions, and hammertoes. Fusion is usually the most successful surgical option for rheumatoid arthritis. However, people need to keep in mind that there are some risks associated with these surgeries.
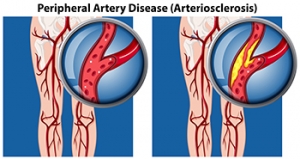
Causes and Diagnosis of Peripheral Artery Disease

Peripheral artery disease, or PAD, poses significant challenges for foot health, stemming from restricted blood flow to the lower extremities. This condition, often caused by atherosclerosis, involves the buildup of fatty deposits in the arteries, leading to narrowed or blocked blood vessels. The diminished blood supply to the feet can result in various symptoms, including pain, cramping, numbness, and weakness, particularly during physical activity. Left untreated, PAD can contribute to serious complications such as foot ulcers, infections, and delayed wound healing. Diagnosing PAD typically involves a comprehensive evaluation by a podiatrist. This process includes a thorough medical history review, assessment of risk factors such as smoking and diabetes, and a physical examination focused on evaluating circulation in the legs and feet. Specialized diagnostic tests, such as ankle-brachial index, or ABI measurement, Doppler ultrasound, and angiography, may also be employed to confirm the diagnosis and determine the extent of arterial blockages. If you are experiencing any of the foot symptoms mentioned above, it is suggested that you consult a podiatrist who can accurately diagnose and offer relief solutions for PAD.
Peripheral artery disease can pose a serious risk to your health. It can increase the risk of stroke and heart attack. If you have symptoms of peripheral artery disease, consult with one of our podiatrists from Princeton Foot and Ankle Associates. Our doctors will assess your condition and provide you with quality foot and ankle treatment.
Peripheral artery disease (PAD) is when arteries are constricted due to plaque (fatty deposits) build-up. This results in less blood flow to the legs and other extremities. The main cause of PAD is atherosclerosis, in which plaque builds up in the arteries.
Symptoms
Symptoms of PAD include:
- Claudication (leg pain from walking)
- Numbness in legs
- Decrease in growth of leg hair and toenails
- Paleness of the skin
- Erectile dysfunction
- Sores and wounds on legs and feet that won’t heal
- Coldness in one leg
It is important to note that a majority of individuals never show any symptoms of PAD.
Diagnosis
While PAD occurs in the legs and arteries, Podiatrists can diagnose PAD. Podiatrists utilize a test called an ankle-brachial index (ABI). An ABI test compares blood pressure in your arm to you ankle to see if any abnormality occurs. Ultrasound and imaging devices may also be used.
Treatment
Fortunately, lifestyle changes such as maintaining a healthy diet, exercising, managing cholesterol and blood sugar levels, and quitting smoking, can all treat PAD. Medications that prevent clots from occurring can be prescribed. Finally, in some cases, surgery may be recommended.
If you have any questions, please feel free to contact our offices located in Princeton, and West Windsor, NJ . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Peripheral Artery Disease
Peripheral artery disease (PAD), or peripheral arterial disease, is a circulatory problem in which there is a reduction of blood flow to the limbs due to narrowed arteries. When peripheral artery disease develops, the extremities do not receive enough blood flow; this may cause symptoms to develop such as claudication, or leg pain when walking. The legs are the most common site of peripheral artery disease.
Claudication, or leg pain when walking, is one of several symptoms that can develop due to peripheral artery disease. Other symptoms caused by the disease include painful cramping in the hips, thighs, or calves after certain activities; leg numbness or weakness; coldness in the lower leg or foot; sores on the lower extremities that do not heal; hair loss on the lower extremities; and a missing or weak pulse in the lower extremities. In more severe cases, pain may even occur when the body is at rest or when lying down.
Peripheral artery disease is typically caused by atherosclerosis, a condition in which fatty deposits build up in the arterial walls and reduce blood flow. Smoking, diabetes, obesity, high blood pressure, and high cholesterol are some of the risk factors for peripheral artery disease.
If you are experiencing pain, numbness, or other symptoms in the lower extremities, see your healthcare professional immediately. Diagnosed peripheral artery disease can be treated with various medications, angioplasty and surgery, exercise programs, or alternative medicine. It is important to consult a healthcare professional to determine the best treatment for you.
Why Live with Pain and Numbness in Your Feet?
Surgical Options for Ingrown Toenails
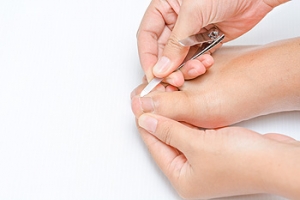
 For persistent or severe ingrown toenails that do not respond to conservative treatment, surgical options offer alternative solutions. One common procedure is a partial nail avulsion. In this procedure, a podiatrist, or foot doctor, removes the part of the nail that is digging into the skin. They may apply a chemical called phenol to the nail bed to prevent that portion of the nail from growing back, reducing the chance of recurrence. In recurrent cases, a total nail avulsion might be necessary, which involves the removal of the whole nail. These procedures are typically performed under local anesthesia in a podiatrist's office, allowing for quick recovery time and minimal disruption to daily activities. Surgical intervention not only resolves the pain and infection associated with an ingrown toenail but also helps prevent future issues, along with proper nail care and guidance from a podiatrist. If you are struggling with persistent ingrown toenails, it is suggested that you make an appointment with a podiatrist.
For persistent or severe ingrown toenails that do not respond to conservative treatment, surgical options offer alternative solutions. One common procedure is a partial nail avulsion. In this procedure, a podiatrist, or foot doctor, removes the part of the nail that is digging into the skin. They may apply a chemical called phenol to the nail bed to prevent that portion of the nail from growing back, reducing the chance of recurrence. In recurrent cases, a total nail avulsion might be necessary, which involves the removal of the whole nail. These procedures are typically performed under local anesthesia in a podiatrist's office, allowing for quick recovery time and minimal disruption to daily activities. Surgical intervention not only resolves the pain and infection associated with an ingrown toenail but also helps prevent future issues, along with proper nail care and guidance from a podiatrist. If you are struggling with persistent ingrown toenails, it is suggested that you make an appointment with a podiatrist.
Ingrown toenails can become painful if they are not treated properly. For more information about ingrown toenails, contact one of our podiatrists of Princeton Foot and Ankle Associates. Our doctors can provide the care you need to keep you pain-free and on your feet.
Ingrown Toenails
Ingrown toenails occur when a toenail grows sideways into the bed of the nail, causing pain, swelling, and possibly infection.
Causes
- Bacterial infections
- Improper nail cutting such as cutting it too short or not straight across
- Trauma to the toe, such as stubbing, which causes the nail to grow back irregularly
- Ill-fitting shoes that bunch the toes too close together
- Genetic predisposition
Prevention
Because ingrown toenails are not something found outside of shoe-wearing cultures, going barefoot as often as possible will decrease the likeliness of developing ingrown toenails. Wearing proper fitting shoes and using proper cutting techniques will also help decrease your risk of developing ingrown toenails.
Treatment
Ingrown toenails are a very treatable foot condition. In minor cases, soaking the affected area in salt or antibacterial soaps will not only help with the ingrown nail itself, but also help prevent any infections from occurring. In more severe cases, surgery is an option. In either case, speaking to your podiatrist about this condition will help you get a better understanding of specific treatment options that are right for you.
If you have any questions please feel free to contact our offices located in Princeton, and West Windsor, NJ . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Ingrown Toenails
An ingrown toenail is a nail that has curved downward and grown into the skin. This typically occurs at either the nail borders or the sides of the nail. As a result, pain, redness, swelling, and warmth may occur in the toe. If a break in the skin forms due to the ingrown nail, bacteria may enter and cause an infection in the area; this is typically characterized by a foul odor and drainage.
Ingrown toenails have multiple reasons for developing. In many instances, the condition is a result of genetics and is inherited. The most common cause, however, is improper trimming; cutting the toenails too short forces the skin beside the nail to fold over. An ingrown toenail can also develop due to trauma, such as stubbing the toe, having an object fall on the toe, or participating in activities that involve repeated kicking or running. Wearing shoes that are too tight or too short can also cause ingrown toenails.
Treatment for an ingrown toenail varies between patients and the severity of the condition. In most cases, it is best to see your podiatrist for thorough and proper treatment. After examining your toe, your podiatrist may prescribe oral antibiotics to clear the infection if one is present. Surgical removal of either a portion of the nail or the entire nail may also be considered. In some cases, complete removal or destruction of the nail root may be required. Most patients who undergo nail surgery experience minimal pain afterward and can return to normal activity the following day.
Ingrown toenails can be prevented with proper nail trimming and by avoiding improper-fitting shoes. When cutting the toenails, be sure that you are cutting in a straight line and avoid cutting them too short. Shoes should not be too short or tight in the toe box.
Symptoms and Causes of Sever’s Disease
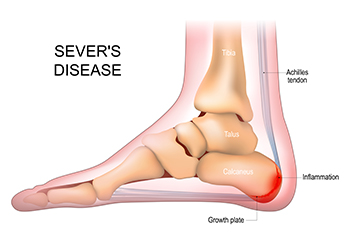
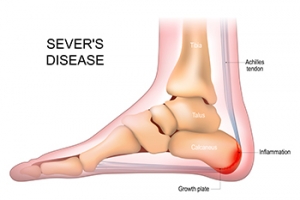
Sever's disease, also known as calcaneal apophysitis, is a heel condition affecting children and adolescents during periods of rapid growth. It occurs when the growth plate at the back of the heel bone becomes inflamed due to repetitive stress or tension from activities like running, jumping, or participating in sports. This condition is not a true disease, but is a temporary condition that typically resolves once the growth plate matures and fuses with the rest of the bone. Symptoms of Sever's disease include heel pain, especially during or after physical activity, limping, and discomfort when pressing on the heel. Factors contributing to its development include overuse or excessive strain on the heel bone, tight calf muscles or Achilles tendon, improper footwear, and biomechanical issues, such as flat feet or high arches. It is suggested that any active child that has heel pain be taken to a podiatrist who can expertly diagnose and treat Sever’s disease.
Sever's disease often occurs in children and teens. If your child is experiencing foot or ankle pain, see one of our podiatrists from Princeton Foot and Ankle Associates. Our doctors can treat your child’s foot and ankle needs.
Sever’s Disease
Sever’s disease is also known as calcaneal apophysitis, which is a medical condition that causes heel pain I none or both feet. The disease is known to affect children between the ages of 8 and 14.
Sever’s disease occurs when part of the child’s heel known as the growth plate (calcaneal epiphysis) is attached to the Achilles tendon. This area can suffer injury when the muscles and tendons of the growing foot do not keep pace with bone growth. Therefore, the constant pain which one experiences at the back of the heel will make the child unable to put any weight on the heel. The child is then forced to walk on their toes.
Symptoms
Acute pain – Pain associated with Sever’s disease is usually felt in the heel when the child engages in physical activity such as walking, jumping and or running.
Highly active – Children who are very active are among the most susceptible in experiencing Sever’s disease, because of the stress and tension placed on their feet.
If you have any questions, please feel free to contact our offices located in Princeton, and West Windsor, NJ . We offer the newest diagnostic and treatment technologies for all your foot and ankle injuries.
Sever's Disease
Sever’s disease, also known as calcaneal apophysitis is a common bone disorder that occurs during childhood. The disease is defined as an inflammation of the growth plate in the heel. When a child has a growth spurt, his heel bone grows faster than the muscles, tendons, and ligaments in his leg. This disease is a result of overuse. The people who are most likely to be affected by this disease are children who are in a growth spurt, especially boys who are from the ages of 5 to 13 years old. 60% of children with Sever’s disease have both heels involved.
Symptoms of this disease are heel pain that intensifies during running and jumping activities. The pain is typically localized to the posterior part of the heel. Symptoms may be severe, and they can easily interfere with daily activities. Children who play soccer, baseball, and basketball are more likely to develop Sever’s disease.
Your doctor will diagnose your child based on his or her symptoms, x-rays are generally not helpful in diagnosing this disease. Your doctor may examine both heels and ask your child questions about his or her activity level in sports. Your doctor may then use the squeeze test on your child’s heel to see if there is any pain. Nevertheless, some doctors might still use x-rays to rule out any other issues such as fractures, infections, and tumors.
Sever’s disease can be prevented by maintaining good flexibility while your child is growing. Another prevention method is to wear good-quality shoes that have firm support and a shock-absorbent sole. Sever’s disease can be treated by ceasing any activity that causes heel pain. You should apply ice to the injured heel for 20 minutes 3 times a day. Additionally, orthotics should be used for children who have high arches, flat feet, or bowed legs.
If you suspect your child has Sever’s disease, you should make an appointment with your podiatrist to have his or her foot examined. Your doctor may recommend nonsteroidal anti-inflammatory drugs (NSAIDs), such as ibuprofen or naproxen to relieve pain. In more severe cases, your child may need a cast to rest his or her heel. Fortunately, Sever’s disease does not cause long-term foot problems. After treatment, your child should start to feel better within two weeks to two months.
How Athletes Cope With Foot Stress Fractures
Athletes face a unique challenge when dealing with foot stress fractures, as these injuries can significantly impact their performance and training routines. The journey to recovery often requires patience, diligence, and a strategic approach. Athletes must prioritize rest and allow ample time for the fracture to heal, refraining from activities that aggravate the injury. Cross-training activities that minimize the impact on the feet, such as swimming or cycling, can help maintain cardiovascular fitness while reducing stress on the injured foot. Additionally, adhering to a balanced diet rich in calcium and vitamin D promotes bone strength and aids in the healing process. Collaborating closely with podiatrists ensures personalized treatment plans tailored to the athlete's specific needs. If you have endured a foot stress fracture from participating in sporting activities or from an injury, it is suggested that you consult a podiatrist who can help you manage this condition.
Activities where too much pressure is put on the feet can cause stress fractures. To learn more, contact one of our podiatrists from Princeton Foot and Ankle Associates. Our doctors can provide the care you need to keep your pain free and on your feet.
Dealing with Stress Fractures of the Foot and Ankle
Stress fractures occur in the foot and ankle when muscles in these areas weaken from too much or too little use. The feet and ankles then lose support when walking or running from the impact of the ground. Since there is no protection, the bones receive the full impact of each step. Stress on the feet can cause cracks to form in the bones, thus creating stress fractures.
What Are Stress Fractures?
Stress fractures occur frequently in individuals whose daily activities cause great impact on the feet and ankles. Stress factors are most common among:
- Runners
- People affected with Osteoporosis
- Tennis or basketball players
- Gymnasts
- High impact workouts
Symptoms
Pain from the fractures occur in the area of the fractures and can be constant or intermittent. It will often cause sharp or dull pain with swelling and tenderness. Engaging in any kind of activity which involves high impact will aggravate pain.
If you have any questions please feel free to contact our offices located in Princeton, and West Windsor, NJ . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.